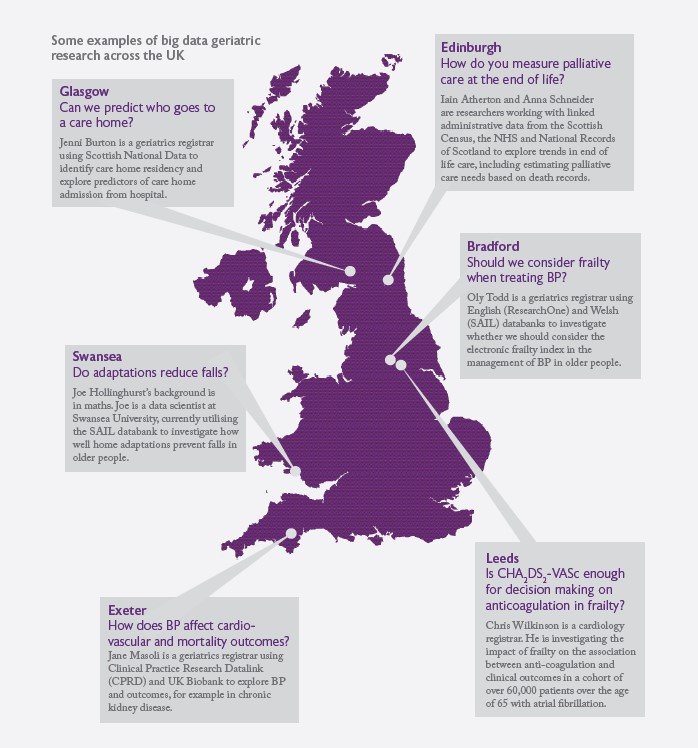
Current state of play
Evidence-based medicine is largely based on clinical trials. These mostly investigate single organ problems, and are used to write single organ guidelines. Yet our patients do not come in neat packages: they are more complex; their priorities diverge; they typically have multiple conditions requiring medications that may interact; and family and social factors are significant influences upon wellbeing but often go unmeasured.
What’s the big idea?
- Primary care records have long been computerised.
- There is recent robust linkage to secondary care datasets.
Benefits and limitations
- It is inclusive: multi-morbidity, frailty, and those lacking capacity are not excluded
- It includes measures used in current practice so findings have easy application
- Data are already available, so less costly
- Can be used to audit the effect of quality improvement strategies
- Data cover a longer period than the typical follow up of a clinical trial
- Large scale allows for high statistical power
- Easier access to data for minority groups, e.g. people with learning disabilities.
- This is a relatively new field, with important methodological challenges to explore
- Lack of positive outcomes: sickness and system-level measures dominate electronic ‘health’ data
- Lack of measures of comprehensive geriatric assessment
- Missing data is not at random, e.g. those who are not accessing services may be at high risk of poor outcomes but will not be captured in routine data.