There is continued uncertainty about how to target suitable recipients in a hospital–wide manner, and what is the most appropriate and cost-effective form of CGA for different settings.
Aim of the project
The overarching aim of this programme of work is to provide high quality evidence to support the delivery of CGA on a hospital wide basis.
Objectives
- The objectives of this proposed integrated research programme are to systematically:
- Define CGA, its processes, outcomes and costs in the published literature
- Identify the processes, outcomes and costs of CGA in existing hospital settings in the UK
- Identify the characteristics of the recipients and beneficiaries of CGA in existing hospital settings in the UK
- Use this new knowledge to develop tools which will assist in the implementation of CGA on a hospital wide basis.
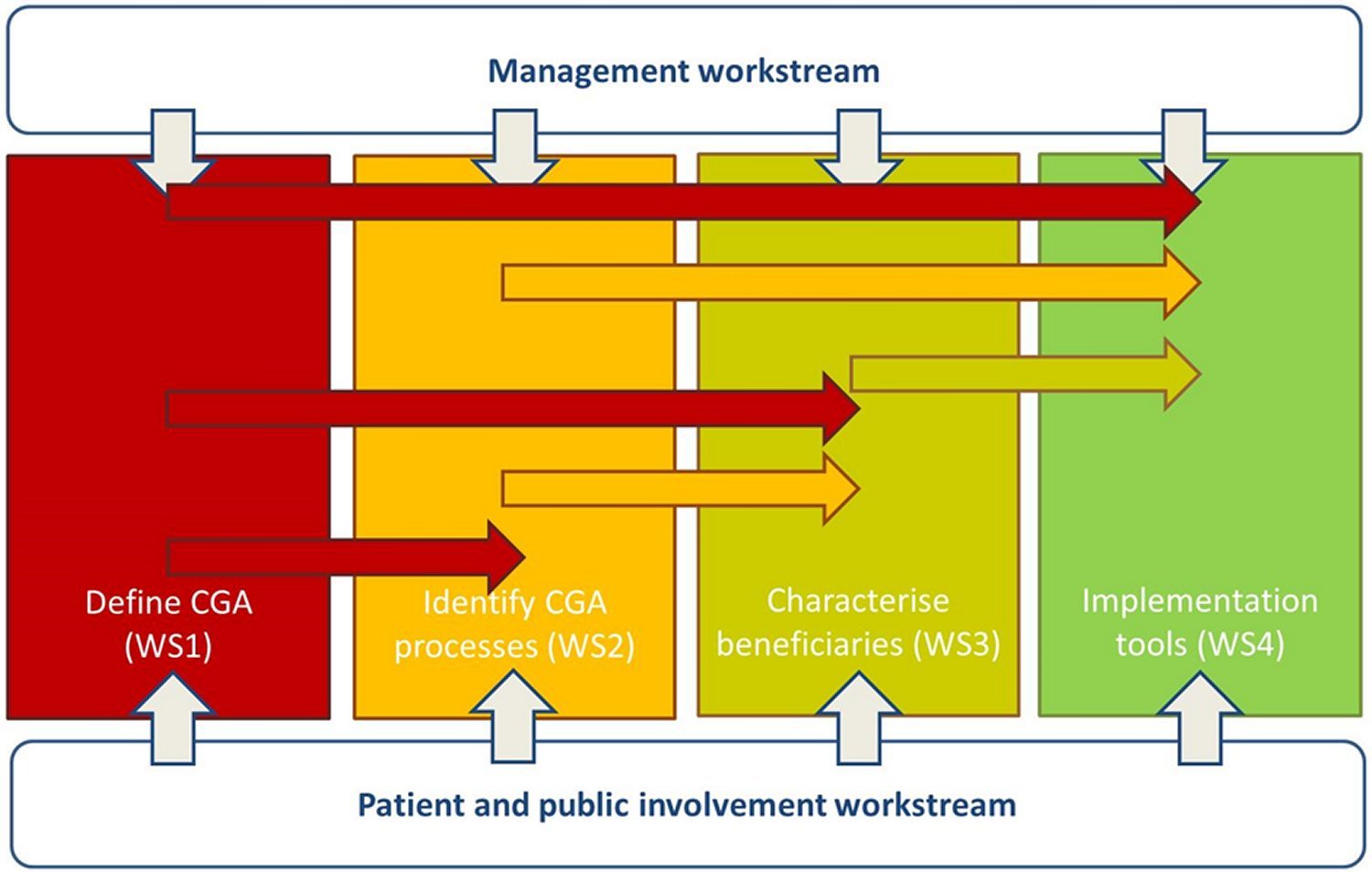
- A diagram of the workstreams that we are using to deliver this programme of work, their interdependencies and relationship to each other is illustrated below.